Free Lactation & Drug Safety Resource List

Author’s Note: This post used to be a static page. I turned it into a blog post to make it more accessible and easier to search. Providing lactation support can be difficult and trying at times – particularly when it comes to medications/herbs and lactation safety and compatibility. There are several great lactation/drug compatibility resources and databases out there but many don’t know where to search or how to access. Compiling all of the evidenced-based resources into one space, so it can be more accessible by not just lactation consultants and those aspiring to be, but also parents and health professionals was the ultimate reason behind the creation of this post.
Do your clients ever call you wondering if a particular medication is compatible with breastfeeding? Many times nursing mothers are told to “pump and dump” or wean by their physicians when in fact, it’s unnecessary. Other times, it’s assumed if a medication is over-the-counter or an herb, it’s completely safe. This is not always the case.
Check below for the most widely used evidence-based resources in order to evaluate drug risk and safety during lactation. This list is arranged by alphabetical order and is by no means exhaustive, so if you’ve found another database or resource helpful, let me know so I can add it.
Questions for lactation professionals and nursing mothers to consider when evaluating risk levels of drugs, herbs, chemicals, etc. during lactation:
1) Will the drug, etc. affect my baby?
2) Will the drug, etc. affect lactation?
3) What are the risks of weaning?
4) What are the options?
For tips on how to counsel your breastfeeding clients on medications, galactagogues and herbs, see these tips by Dr. Frank J. Nice, RPh, DPA, CPHP.
Electronic Databases
Breastfeeding Network – Provides FREE Fact Sheets on a wide array of drugs, medical procedures and health conditions and compatibility with breastfeeding available here. These are great to share with your clients (and to encourage them to print them out and discuss safety concerns or potential alternatives with their health care provider). Also provides a detailed description of an ‘Introduction to the Safety of Drugs Passing Through Breastmilk’ here. For common FAQs concerning breastfeeding and generic medications, see here. Also contains general ‘Information on Breastfeeding’here, ‘Thinking about Breastfeeding’ here, ‘Breastfeeding and Perinatal Mental Health’ here and common ‘Questions about your Baby’here.
TIP: when using drug search databases: Since drug names can differ by country and even more so if it’s a generic vs. name brand drug, if the drug you are searching does not show up in the database search engine, then google that particular drug for the active ingredient and search by that instead.
e-lactancia – Compiled by pediatricians affiliated with APILAM. Uses risk levels 0 (no risk) -3 (very high risk). Covers “medical prescriptions, phytotherapy (plants), homeopathy and other alternative products, cosmetic and medical procedures, contaminants, maternal and infant diseases and more.” For common FAQs concerning lactation and medications, see here. Very easy to use and understand. A great resource to share with families so they can look up their own medications. Available in English and Spanish.
Infant Risk Center – Researched and compiled by Dr. Thomas Hale, PhD and author of the renowned and widely used medical lactation risk and reference guide, ‘Hale’s Medications and Mothers’ Milk.’ This reference guide is updated every 2 years, with the most recent edition published in 2017 and a new edition coming out in 2019). This resource uses lactation risk categories 1 (safest) – 5 (contraindicated). It covers prescription medications, chemicals, herbals, vitamins and radioisotopes/radiocontrast agents. This reference guide is also affiliated with the Infant Risk Center at Texas Tech University Health Sciences Center. A detailed description of ‘Drug Entry Into Human Milk’ is available here. If you have a question regarding a particular drug, you can call a free helpline at (806) 352 – 2519.
Medications & Mother’s Milk is an electronic database also established by Dr. Hale. Annual subscriptions are available at varied prices for individuals and groups/institutions. Mobile apps are also available for both androids and iOS – one is for healthcare professionals ($9.99) and the other is a simplified version for parents ($3.99). You can view options here.
LactMed – Sponsored by the National Institute for Health (NIH)’s US National Library of Medicine TOXNET Toxicology Data Network. It provides peer-reviewed, fully referenced, evidence-based resources. Users can look up lactation risk of both drugs and chemicals. This site is highly medicalized and may be too versed in “medical speak” for the average consumer to fully understand. LactMed also offers a mobile free app for both android and iOS.
MotherRisk – Sponsored by The Hospital for Sick Children in Toronto. It provides evidence-based information about the compatibility of prescription and over-the-counter medications, herbal products, chemicals, radiation, chronic diseases, infections, occupational, environmental, and other exposures during pregnancy and lactation. Also covers general FAQs about medications and lactation. Various brochures are available here. Offers a FREE MotherRisk Hotline: 1-877-439-2744, which is open Monday – Friday 9 a.m. to 12pm and 1 to 5 p.m. Eastern Standard Time.
Additional Drug Safety & Lactation Resources
Breastfeeding & Human Lactation Study Center (which is a part of the Division of Neonatology at University of Rochester Medical Center’s Golisano Children’s Hospital) under the direction of Ruth A. Lawrence, M.D. Healthcare professionals can call (585) 275-0088 at no cost for information on drug risk and compatibility and to consult on difficult breastfeeding issues. Note: This hotline is for healthcare professionals ONLY, not for parents or your breastfeeding clients. For more information, see here. See here for a breastfeeding site geared specifically toward your breastfeeding clients and families.
Cindy Curtis, RNC, IBCLC, CCE, CD of Breastfeeding Online has compiled a comprehensive and beautifully organized list of lactation risk and compatibility with direct links to articles on breastfeeding and alcohol, herbals, epidurals, antidepressants, social drugs, cigarettes, prescription and non-prescription drugs and more. This is an accessible and quite handy resource to share with your breastfeeding clients or lactation specialists-in-training.
Frank J. Nice, RPH, DPA, CPHP of Nice Breastfeeding has written several books on medications and compatibility with breastfeeding: ‘Nonprescription Drugs for the Breastfeeding Mother’ (2017) here. ‘Recreational Drugs and Drugs Used to Treat Addicted Mothers: Impact on Pregnancy and Breastfeeding’ (2016) available here. ‘The Galactagogue Recipe Book’ (2017) which discusses dosage, uses, and cautions of galactogogues here. There are free downloadable pdfs on a wide array of lactation and drug risk categories including herbs and galactagogues, recreational drug use and Domperidone are available here. Free patient resources with helpful links are available here. You can find information for healthcare providers on how to counsel breastfeeding mothers who have drug-related questions here.
International Breastfeeding Centre established by Dr. Jack Newman, MD, IBCLC provides a general overview of maternal medications and breastfeeding in a Q&A blog post format, addressing general FAQs, whether or not to continue breastfeeding, how drugs get into breast milk and lactation compatibility with specific medications here. If you have a question about a particular drug’s compatibility with breastfeeding (or you’re dealing with a difficult breastfeeding case in general and would like some guidance and feedback), Dr. Newman answers emails from Lactation Specialists at no charge here. Information sheets on a wide array of lactation topics are available here, many of which are translated into different languages here.
Kelly Bonyata, BS, IBCLC of Kellymom has compiled lists of lactation risk databases in English and other languages, common FAQs on specific drugs, treatments and medical procedures, lactation risk resources and a detailed list of reference links here.This is an accessible, easy to understand resource to share with your breastfeeding clients.
La Leche League International (LLLI) has also published some articles and FAQ fact sheets on medications and breastfeeding. It also has a comprehensive resource of hyperlinked articles addressing breastfeeding with maternal illness, conditions, diseases and if medications/treatments are compatible. LLLI’s site, including it’s articles (typically written for mothers and parents by mothers (who are also breastfeeding counselors), are fantastic reat resources to share with nursing mothers and families as they are easily accessible, usually short and sweet, and written for an audience without a medical background. Just click on the title(s) below:
Wendy Jones, BSc, MSc, PhD, MRPharmS of Breastfeeding and Medication.This comprehensive site includes free downloadable Fact Sheets, evidence-based useful links on medication and breastfeeding, E-Learning Packages/Training Packs, aimed at GPs (latest cost was £40.00), which can be purchased here. She has also authored the books, “Breastfeeding and Medication.” (2018) and “Why Mothers’ Medication Matters” (2017).
Herbs & Breastfeeding
Kelly Bonyata, BS, IBCLC of kellymom.com has created a simple, accessible resource list of specific herbals and natural treatment and compatibility with lactation here. For information on marijuana and breastfeeding, see here. These are both fantastic, easy to read and understand resources to share with your breastfeeding clients.
Sheila Humphrey, BSc, RN, IBCLC has written the ‘The Nursing Mother’s Herbal’ (2003) available here, which discusses the effects of a wide array of herbs, dietary supplements and natural remedies on lactation and lactation-related maladies such as mastitis, plugged ducts, thrush and more. Her book is organized into Herb Safety Categories A (no contraindications) – E (Avoid. Toxic plant with no justifiable medical use). See here for a more thorough description of the Herb Safety Categories and see here for a review of her book from LLLI.
 This list is by no means exhaustive. If you have a evidence-based resource on drug safety and lactation that you recommend and it’s not included in the list, then please, send me a message with a description and relevant info so that I can include it. Thanks a bunch, xx
This list is by no means exhaustive. If you have a evidence-based resource on drug safety and lactation that you recommend and it’s not included in the list, then please, send me a message with a description and relevant info so that I can include it. Thanks a bunch, xx






 Do you have an idea for Galactablog’s FREEBIE Week? Don’t be shy! Please do share – I promise to give you full credit. If you’re a company, private practice, clinic, hospital, non-profit, non-governmental organization, etc. and have a FREE opportunity, resource or item that you’d love offer to Galactablog readers, drop me a line. As long as you are WHO Code Compliant, you’ll be given full consideration. You can contact me
Do you have an idea for Galactablog’s FREEBIE Week? Don’t be shy! Please do share – I promise to give you full credit. If you’re a company, private practice, clinic, hospital, non-profit, non-governmental organization, etc. and have a FREE opportunity, resource or item that you’d love offer to Galactablog readers, drop me a line. As long as you are WHO Code Compliant, you’ll be given full consideration. You can contact me 

 Next up, how about
Next up, how about 





 Dr. Frank Nice
Dr. Frank Nice





 This list is by no means exhaustive. If you have a evidence-based resource on drug safety and lactation that you recommend and it’s not included in the list, then please, send me a message with a description and relevant info so that I can include it. Thanks a bunch, xx
This list is by no means exhaustive. If you have a evidence-based resource on drug safety and lactation that you recommend and it’s not included in the list, then please, send me a message with a description and relevant info so that I can include it. Thanks a bunch, xx








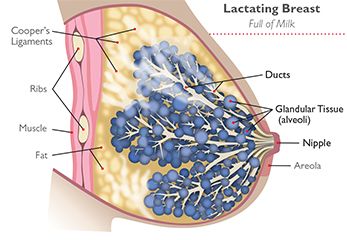

 closely (and use your imagination), that in a bunch of grapes, you can point out the ducts, alveoli (clusters of glandular tissue that look like small, grape-like sacs), lobules (cluster of alveoli), a lobe (cluster of lobules), ductules, adipose (fatty) tissue and so on? Get creative and have fun with it – I guarantee they’ll pay attention. Now if you happen to come up with a simple, basic, quick script, please do share – mine is still kinda rambly and dense, it’s something I’m constantly evolving.
closely (and use your imagination), that in a bunch of grapes, you can point out the ducts, alveoli (clusters of glandular tissue that look like small, grape-like sacs), lobules (cluster of alveoli), a lobe (cluster of lobules), ductules, adipose (fatty) tissue and so on? Get creative and have fun with it – I guarantee they’ll pay attention. Now if you happen to come up with a simple, basic, quick script, please do share – mine is still kinda rambly and dense, it’s something I’m constantly evolving.